Abstract
To explore if change in the extent of emphysema correlated with change in lung function, the effect of resection of emphysematous tissue was studied by computed tomography (CT) densitometry. In addition, the current authors studied how surgery-induced change in emphysema related to lung density in control subjects.
In total, 30 patients (14 females; mean±sdage 59±10 yrs) with severe emphysema before and 3 months after lung volume reduction surgery (LVRS), 48 patients with moderate emphysema and 76 control subjects were investigated. Lung density (15th percentile point) of both lungs and heterogeneity of lung density between 12 isovolumetric partitions in each lung were calculated from chest CT images.
The 15th percentile point and its heterogeneity could distinguish controls from subjects with moderate emphysema with a sensitivity and specificity of >95%. LVRS significantly increased lung density by 5.0±10.9 g·L−1(n = 30). Improvement in the diffusing capacity of the lung for carbon monoxide and in residual volume significantly correlated with an increase in lung density (n = 20 and 28, respectively). Change in forced expiratory volume in one second did not correlate with change in lung density.
In conclusion, lung density 15th percentile point is a valuable surrogate marker for detection of both the extent of and reduction in emphysema.
The diagnosis of emphysema is most reliably obtained by pathological examination of lung tissue and is defined by airspace enlargement beyond the terminal respiratory bronchioli1,2。Shortly after the invention of computed tomography (CT) by Sir G. Hounsfield in 1972, it became obvious that lung densitometry had the potential to quantify lung density in various diseasesin vivo, including emphysema3。不同的参数,如平均肺密度,relative area or density mask and percentile point have been introduced for the quantification of lung density in patients with emphysema4–6。These parameters have been validated against pathology4–6, pulmonary function tests6,7and health status8。A minor effect of age on lung density in healthy individuals has been shown in a cross-sectional study9。The results of these cross-sectional studies suggest that lung density measurements may be useful for the detection of progression of emphysema and possibly for monitoring the effect of therapeutic interventions.
Three longitudinal studies on emphysema, associated with PiZZ α1-antitrypsin deficiency, were able to show changes in the 15th percentile point as an indicator of disease progression10–12。The latter studies took >2 yrs and it was difficult to demonstrate a correlation between change in lung density and change in lung function parameters. Only recently has this been accomplished, with forced expiratory volume in one second (FEV1) in a 4 yr study of density analysis of the upper zone of the lungs12。In contrast, lung volume reduction surgery (LVRS) for emphysema offers an opportunity for short-term study of changes in the extent of emphysema13。Rather than measure progression of disease, LVRS makes it possible to study whether reduction in the amount of emphysematous tissue results in a shift in both lung density and lung function in the direction towards normal values. To be able to evaluate this shift, a set of lung density values of a population with normal lungs is needed but this is not as generally available as for lung function tests. Furthermore, a short-term intervention, such as LVRS in patients with emphysema, allows the study of whether changes in lung function and lung density correlate. Such a finding may facilitate acceptance of densitometry as a surrogate marker for studies on emphysema. The aim of the present study was to measure lung density in patients with severe pulmonary emphysema before and 3 months after LVRS and to study the association with changes in lung function.
METHODS
Subjects
To distinguish between normal and emphysematous lungs, CT-densitometry was first performed in individuals with normal lung function and patients previously diagnosed with pulmonary emphysema. Individuals with normal lungs were identified by a radiologist, who screened for normal radiological appearance of the lungs using a chest CT. The patients were from the Dept of Orthopaedic Surgery (Leiden University Medical Center (LUMC), the Netherlands) and were screened for the presence of pulmonary metastases before surgical treatment of osteosarcoma. CT images of the chest were only used for lung densitometry when images had a normal radiological appearance and both spirometry and diffusing capacity of the lung for carbon monoxide (DL,CO) of the patients were within 1.64sdof the normal predicted value, as defined by the European Respiratory Society (ERS) standards14。
A second set of patients, with a known diagnosis of smoking-related emphysema at the Pulmonary Outpatient Clinic of LUMC, volunteered to participate in the study for a CT scan and lung function measurements.
A third set of patients consisted of patients who were referred to Leiden or Zurich (Switzerland) for bilateral video-assisted thoracoscopic LVRS. The patients were investigated by CT and lung function prior to surgery and 3 months thereafter. Patients with nonbullous pulmonary emphysema were included when they were severely symptomatic despite optimal medical therapy, had severe airflow obstruction (FEV120–40% predicted) and pulmonary hyperinflation (residual volume (RV) >200% pred, RV/total lung capacity ratio >0.6). Exclusion criteria were severely impairedDL,CO(<20% pred) and significant coronary artery disease. All patients had undergone rehabilitation at other institutions before referral. LVRS was performed by means of bilateral, video-assisted, stapled resection of ∼30% of lung volume. By means of analysis of the CT scans and perfusion scintiscans, target areas were identified as the lung zones with the most pronounced emphysematous alteration and the greatest reduction in perfusion13。In addition, target areas were selected on the basis of visual observation of areas with delayed resorption atelectasis during the surgical intervention13。All subjects included were asked to participate in the present study and gave written informed consent. Approval for the study was obtained from the Ethical Boards of LUMC and University Hospital Zurich.
Lung function
In both centres spirometry and assessment of lung volumes andDL,COwere performed in a standardised manner14,15。
CT
Spiral CT scan was performed at LUMC using a Phillips AVE-U scanner (Phillips Medical Systems, Eindhoven, the Netherlands) at 140 kVp, 40 mAs, pitch factor 2, 7 mm collimation, reconstructed with a slice thickness of 7 mm, 5 mm increment and reconstruction filter 416。At the University Hospital Zurich, patients were scanned using a Siemens Volume Zoom multi-slice CT (Siemens GmbH, Erlangen, Germany) using an acquisition protocol of 140 kVp, 40 mAs, pitch factor 1.5, 5 mm collimation, reconstructed with a slice thickness of 5 mm, 2.5 mm increment and reconstruction filter B10. All patients were scanned with the instruction to hold their breath at full inspiration. Reconstruction algorithms remained the same during the study period. CT calibration was performed as recommended by the manufacturer16。
Densitometry
The CT scanner is able to determine a range of different densities present in both lungs. The frequency of each of these densities can be expressed in a histogram and analysed in various ways. The present authors proposed the use of the percentile point method (fig. 1⇓).This method defines the 15th percentile point as the density value represented on the x-axis for which 15% of all pixels in the density histogram have a lower density. It can be applied to individuals with healthy lungs and to patients with mild-to-severe emphysema. In the assessment of emphysema, it has been shown that the percentile points between the 10th and 20th percentile are equally sensitive, with an optimum at approximately the 12th percentile10。In practice, the 15th percentile point is used.
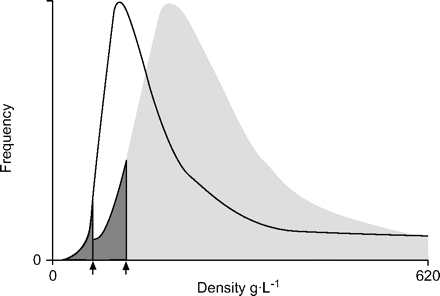
Density distribution in the lung. Histogram of densities from a subject with normal lungs (░) and a patient with emphysema (––––). The 15th percentile point (▒) is the density value on the x-axis that covers 15% of all densities of the histogram. ↑: 15th percentile point.
The 15th percentile point (Perc15) of both lungs was measured, as well as the CT-predicted surface area to volume, as presented by Coxsonet al.6, using semi-automated computer software (Pulmo-CMS; Medis Specials, Leiden, the Netherlands)16。
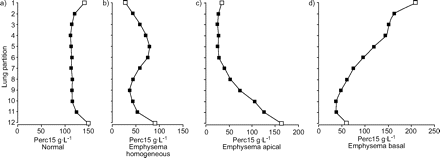
The software is able to measure air density in the images outside the patient and blood density in the abdominal aorta in the patient, with both being used fora posterioricalibration16。In both lungs, the density in 12 partitions was measured, with equal volumes from the top of the lung down to the base. Out of the 12 partitions, the top and basal partitions were excluded from analysis to prevent influence by partial volume effects. Next, Perc15 was measured in each of the remaining 10 partitions and the mean Perc15 was calculated. Subsequently, thesdof these Perc15 values was considered the heterogeneity of emphysema (fig. 2⇓).
Example graphs of apical and basal localisation of emphysema showing the heterogeneity of densities present in single patients. Out of the 12 lung partitions of equal volume, the top and basal partitions were excluded from analysis (□) to prevent influence by partial volume effects. In a) lung density of a normal patient at the 15th percentile point (Perc15) is measured in all 10 partitions from lung top (apex; partition 1) to base (partition 12) showing almost similar Perc15 values (▪) in each partition; the mean Perc15 is 120 g·L−1。Therefore, heterogeneity, defined as theSDof the 10 Perc15 values, is low (3.8 g·L−1).In b) a homogeneous distribution of Perc15 in a patient with emphysema is shown. The mean Perc15 of 10 partitions is 35.5 g·L−1and the heterogeneity is 15 g·L−1。In contrast, graphs c) and d) show two different patients with heterogeneous types of emphysema. In c) the emphysema is predominantly located in the apex; the mean Perc15 in all 10 partitions is 34.1 g·L−1and heterogeneity is 36.7 g·L−1。In d) the emphysema is predominantly located in the base of the lungs; the mean Perc15 of all 10 partitions is 68.6 g·L−1and the heterogeneity is 48.5 g L-1.
Statistical analysis
Results are presented as mean±sd。Statistical significance was determined with paired and unpaired t-tests. The Kolmogorov-Smirnoff analysis showed that none of the baseline parameters had a non-Gaussian distribution.
The ability of densitometry to predict the presence of emphysema in a combined set of data from controls and emphysema patients is defined previously, with Perc15 and heterogeneity as independent variables. Spearman correlations were calculated between change in lung density parameters, change in CT-lung volumes and change in absolute values of the lung function parameters FEV1, RV andDL,CO。
RESULTS
Densitometry in normal and emphysematous lungs
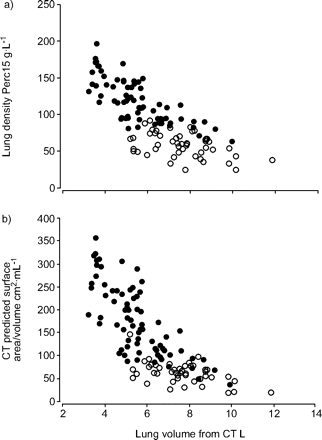
Perc15 was determined in subjects with normal lungs and in patients with emphysema. Baseline patient characteristics are shown in table 1⇓。For both study populations, figure 3a⇓shows the relationship between lung density and lung volume and can be compared with the CT-predicted surface area to volume, and figure 3b⇓shows the relationship to lung volume. Between the two groups some overlap in densities occurred. From pathological information, it is known that emphysema can have variable distribution throughout both lungs, producing a heterogeneous density distribution. The current authors found that the heterogeneity of emphysema, represented by the variability in Perc15, ranged 2–18 g·L−1and 5–50 g·L−1in patients with normal lungs and patients with emphysema, respectively (fig. 4⇓).Logistic regression demonstrated that the presence of emphysema in the aforementioned groups can be predicted by density Perc15 with a sensitivity of 92% and a specificity of 97%. For CT-predicted surface to volume the sensitivity and specificity were 88 and 93%, respectively. By also considering the density Perc15 heterogeneity in the analysis, the sensitivity and specificity improved to 98 and 100%, respectively.
Lung density in subjects with normal lungs (•) and in patients with emphysema (○). a) Relationship between lung density 15th percentile point (Perc15) and computed tomography (CT)-derived lung volume of subjects with normal lungs and patients with emphysema. b) CT-predicted surface area to volume and its relationship to lung volume in the same subject groups. Images were taken at breath-hold after the instruction to inhale to total lung capacity.
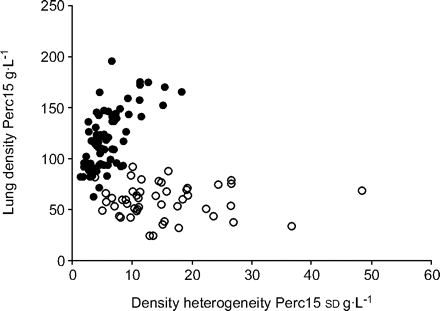
Relationship between lung density and density heterogeneity of the 15th percentile point (Perc15). Heterogeneity of emphysema is represented by the variability in Perc15 related to whole lung density expressed as Perc15. Heterogeneity was calculated as thesdof Perc15 values present in 10 partitions. •: control subjects; ○: patients with emphysema.
Baseline patient characteristics
Densitometry in LVRS for emphysema
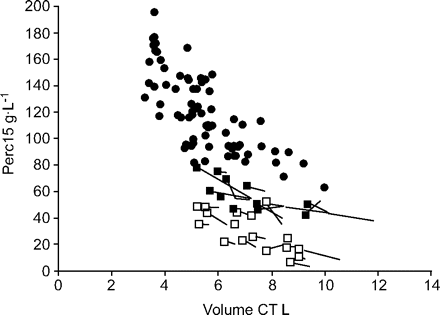
Baseline patient characteristics of the LVRS group are shown in table 1⇑。These patients represented a different population from that shown in figure 3⇑。LVRS resulted in an increase in lung density Perc15 of 5.0±10.9 g·L−1(n = 30; p = 0.01). The effects of LVRS are summarised in table 2⇓。The data points in figure 5⇓show, on average, an increase in lung density in the direction of density values for normal subjects. CT-measured lung volume changed on average by 0.94±1.14 L after surgery (n = 30; p = 0.001; fig. 5⇓).肺气肿病人一家的异质性r to surgery was 8±11 g·L−1and did not change significantly after the intervention.
Change in lung density in patients with emphysema. Relationship between lung density and computed tomography (CT)-derived lung volume of subjects with normal lungs (•) and patients with emphysema who had surgical treatment in order to reduce the severity of emphysema. ▪: patients from Leiden, the Netherlands; □: patients from Zurich, Switzerland. Each line represents a patient, and the beginning and end of the lines (with ▪ or □ at the end) indicate the pre-operative Perc15 value and the post-operative value of lung density, respectively. The 15th percentile point (Perc15) increased on average by 5.0±10.9 g·L−1(n = 30, p = 0.01), parallel to the relationship between lung density and lung volume.
Summary of lung volume reduction surgery effects
Correlation between change in lung density and change in lung function
There was a significant correlation between change inDL,COand change in lung density in subjects who had surgery (r = 0.56; p = 0.009; n = 20; fig. 6⇓).In total, 10 subjects could not perform aDL,CO根据人g调动足够的质量uidelines either before or after treatment. Change in lung volumes, such as total lung capacity and RV, correlated with change in density (r = -0.51, p = 0.005, n = 28 and r = -0.54, p = 0.003, n = 28, respectively). Change in FEV1或FEV1/forced vital capacity did correlate with change in lung density (r = 0.24, p = 0.19 and r = 0.26, p = 0.23). The change in FEV1only correlated significantly with the change in residual volume (r = -0.57; p = 0.001; n = 28).
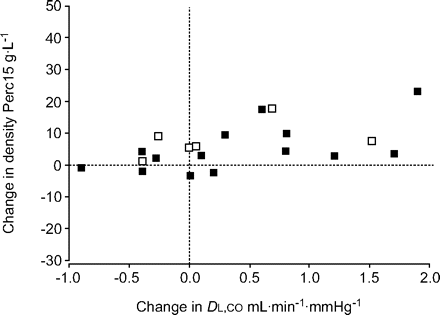
Relationship between change in lung density and change in lung function. Correlation between change in lung density and change in lung diffusion capacity in lung volume reduction surgery patients. Not all 30 patients could perform a diffusing capacity of the lung for carbon monoxide (DL,CO) manoeuvre according to European Respiratory Society guidelines. □: patients from Leiden; ▪: patients from Zurich. r = 0.56, p = 0.009, n = 20.
DISCUSSION
本研究的目的是评估茶nge in lung density caused by LVRS in patients with severe centrilobular emphysema and to study whether removal of severely affected emphysematous tissue changes lung density in association with changes in lung function, such as FEV1, lung volumes andDL,CO。The current study demonstrated that lung density increased after surgery and that changes inDL,COand RV correlated positively with changes in lung density. Previous studies have repeatedly shown high cross-sectional correlations between pathology scores of emphysematous tissue and lung density4–6。In contrast, a few longitudinal studies were able to show changes in lung density as indicators of disease progression11,12。The presentin vivoobservations confirm results of a phantom study that showed changes in density could be measured accurately by CT-derived densitometry17。To the present authors’ knowledge, no study has previously shown a correlation between change inDL,CO或FEV1and change in lung density in centrilobular emphysema18。Only a correlation with change in exercise capacity has been reported19。Previously, the current authors calculated the sensitivity to detect change in Perc15 and change in lung function in panlobular emphysema, and reported that Perc15 was two-fold more sensitive in detecting progression of disease than lung function11。The authors have now shown that emphysema in subjects with panlobular emphysema is not the only group of patients in which lung density is a meaningful measurement; it can also be of value in subjects with general chronic obstructive pulmonary disease (COPD) and centrilobular emphysema.
Lung density was measured in patients with healthy lungs as defined by clinical radiologists and based on normal values of both spirometry andDL,CO。Detailed analysis showed that the density of the lung is dependent on the volume of inhaled air present in the lungs during scanning. Remarkably, in healthy lungs of large volume (fig. 3a⇑), no high densities were observed, suggesting that lung density is dependent on the anatomical size of the lungs. Gevenoiset al.9suggested that the relationship between density and lung volume in normal subjects indicated a lower amount of alveolar tissue per unit of volume in larger lungs and a higher amount in smaller lungs, based on the observation that the structure of the alveolar wall is unrelated to the lung size. Future work is needed to establish if this is the only explanation for the observed absence of values (fig. 3a⇑).
It has been reported that radiological (semi-)quantitative assessment may reveal unequal distribution of emphysema between the top and base of the lung, as well as between the left and right lung20,21。The current authors’ method for assessment of Perc15 and heterogeneity of emphysema was quantitative and able to distinguish normal from emphysematous lung in the selected population. Analysis of heterogeneity of whole lung density may contribute to solving the fairly widespread disagreement about the precise separation of fully expanded normal lung from early emphysema22。
然而,一些限制适用于目前的斯图dy. The lung densities found in the patients from Zurich were on average lower than those from Leiden. This is likely to be caused by differences in the type of CT scanners and differences in reconstruction algorithms. While inter- and intra-scanner variability can be reduced by recalibration within the images, intra-subject variability is highly influenced by the relationship between volume of air in the lungs and density. The current authors felt that correction for the difference in lung volume between individuals during scanning was not adequate. Confounder analysis showed that if density is corrected for volume in a cross-sectional study, a dependency is introduced between the corrected density and body weight (B.C. Stoel, Dept of Radiology, LUMC; unpublished data). As body weight may be influenced by emphysema, this dependence becomes an unacceptable confounding factor.
The National Emphysema Treatment Trial in the USA identified that the site of lung tissue most affected by emphysema is of prime importance to the outcome of LVRS23。The study patients were selected for surgery when marked upper lobe emphysema was present, with relatively preserved lung tissue (lung density) in the rest of the lungs. Before surgery, the heterogeneity of Perc15 was rather wide and was not significantly changed after surgery. It has been postulated that in heterogeneous emphysema, compression of the spared lung by the diseased areas leads to focal hypoventilation and subsequent underestimation of gas exchange24。The absence of change in heterogeneity by surgery in the current study may indicate that lung tissue in the post-surgical assessment had the same distribution of tissue densities, suggesting that lung tissue was not expanded in a different manner as compared with the pre-surgical period. This was also observed by radiological assessment of the CT images. In all of the study patients, the diaphragm was shifted upwards to replace the surgically removed emphysematous tissue. Apparently, the remaining lung tissue was expanded with preservation of heterogeneity of Perc15, but more advanced analysis of local changes in the lung is needed to study this change in heterogeneity in more detail.
In conclusion, the present study demonstrated that changes in the extent of emphysema can be detected by lung densitometry, further validating densitometry as a surrogate outcome parameter for the treatment of emphysema.
Acknowledgments
J. Stolk and B.C. Stoel were supported by grants from the Fifth Framework Program of the European Commission (Project No. QLG1-2000-01752). E.W. Russi was supported by the Swiss Science Foundation.
The authors would like to thank A.H.M. Taminiau (Dept of Orthopaedic Surgery, Leiden University Medical Center, Leiden, the Netherlands) for the help with recruitment of patients, J. Lenssen for critical reading of the manuscript and council members of the Alpha1 International Registry (www.aatregistry.org) for helpful discussions.
Footnotes
For editorial comments see page 1075.
- ReceivedApril 26, 2006.
- AcceptedFebruary 17, 2007.
- © ERS Journals Ltd